Soft Cast Contraindications and Common Application Errors
Soft casting (semi-rigid immobilization) can provide excellent support while preserving controlled movement—when properly indicated and correctly applied. But in the wrong situation, or with poor technique, outcomes can worsen: pain, skin injury, instability, and delayed healing. This guide reviews soft cast contraindications and the most common application errors, offering a practical safety checklist for clinical use.
Key principle: soft cast does not replace diagnosis and clinical decision-making
Soft cast is a tool—not an automatic solution. Accurate diagnosis and stability assessment must come first, including fracture risk, neurovascular status, and tissue condition. Many failures happen when soft cast is selected simply for comfort, despite the need for rigid immobilization.
Contraindications for soft cast
Contraindications can be divided into absolute (do not use) and relative (use only with strict caution and clinician oversight).
Absolute contraindications
- Unstable or displaced fractures: inadequate stabilization increases displacement risk.
- Severe ligament injuries with clear instability (e.g., Grade III sprains): often require rigid immobilization or specialized bracing.
- Suspected compartment syndrome: disproportionate pain, pain with passive stretch, progressive swelling—medical emergency.
- Major neurovascular compromise: coldness, pallor/cyanosis, worsening numbness or weakness.
- Active infection or large open wounds under the cast area: higher infection risk and limited monitoring.
Relative contraindications
- Marked fluctuating swelling in the first 24–72 hours: higher risk of becoming too tight or too loose.
- Highly sensitive skin or contact dermatitis history: possible resin or underlayer sensitivity.
- Low adherence risk: children or patients likely to pick, scratch, or violate restrictions.
- High-risk comorbidities: uncontrolled diabetes, peripheral vascular disease, neuropathy—requires closer monitoring.
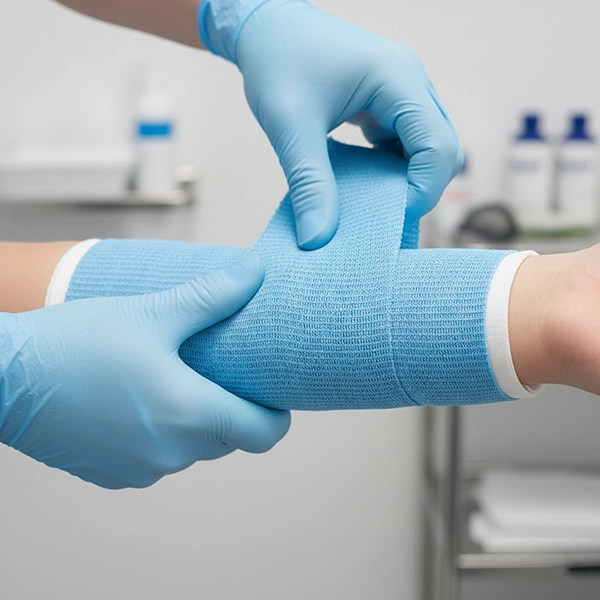
Common application errors and their consequences
Most technique errors fall into three categories: tension, overlap/thickness, and molding/joint positioning. Each mistake can lead either to excessive pressure and pain or to looseness and poor stabilization.
1) Excessive tension (Over-tension)
- Signs: throbbing pain, tingling/numbness, coldness or color change, distal swelling.
- Causes: pulling too hard, high tension over bony prominences, ignoring early swelling.
- Fix: controlled uniform tension; reduce tension over prominences; early follow-up.
2) Insufficient tension (Under-tension)
- Signs: unwanted motion, slipping/loosening, mechanical pain, weak support.
- Causes: fear of tightening, inadequate overlap, wrong roll size/length.
- Fix: tension until wrinkle-free; 30–50% overlap; correct sizing.
3) Uneven overlap and pressure lines
- Signs: ridges, focal pain, blisters, redness/sores along a line.
- Causes: overlap below 30% in segments or excessive buildup.
- Fix: maintain consistent overlap; adapt technique at high-contour joints.
4) Fingertip molding
A very common mistake is shaping with fingertips, creating hotspots and skin injury.
- Fix: mold using open palms with distributed pressure.
5) Incorrect joint position during application
- Ankle: plantarflexed immobilization can delay gait and rehab.
- Wrist: excessive flexion/extension leads to pain and functional limitation.
- Thumb: poor spica alignment reduces ligament support.
Fix: maintain functional neutral positioning until setting is complete.
6) Poor water-activation timing
- Too warm: very short working time, insufficient molding.
- Over-soaking: over-activation makes handling difficult.
- Fix: lukewarm water, short dip, gentle squeeze.
7) Lack of patient education
Many complications happen after leaving the clinic. Without clear instructions, patients may delay seeking help.
- No objects under the cast
- Keep it dry; avoid sand/dirt ingress
- Know red flags: escalating pain, numbness, color change, odor, discharge

Quick safety checklist (before discharge)
- CSM check: Color, Sensation, Motion
- No focal pressure over bony prominences
- Uniform overlap and soft edge finishing
- Home-care and red-flag education
- Early follow-up scheduled (often within 3–7 days)
Conclusion
Soft cast is highly useful—but not for every patient and not in every scenario. Respecting contraindications and avoiding common technique errors is the difference between safe recovery and preventable complications. With correct indication and standardized application, soft cast can offer strong support with improved comfort.
Call to Action
Explore fiberglass cast products suitable for semi-rigid clinical applications:
View Fiberglass Cast Products


