Skin Safety: Resin Allergy & Contact Dermatitis with Fiberglass Casts
Most patients tolerate fiberglass casts well, yet a minority may develop resin-related irritation/allergy or contact dermatitis. Risk awareness, proper material selection (padding, edge tape), sound technique, and patient education are the pillars of prevention and timely management. This practical guide covers red flags, likely causes, prevention protocols, a clinical playbook, and home-care advice to maximize skin safety with fiberglass casting tapes (synthetic cast bandages).
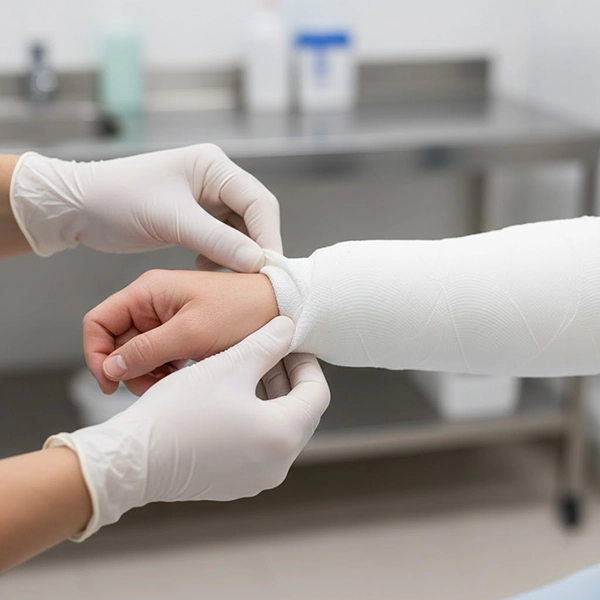
1) Resin irritation vs. contact dermatitis
- Resin-related irritation/allergy: diffuse erythema, burning, or generalized itch, often peaking in the first hours/days. Moist skin contacting activated resin or excess activation water can contribute.
- Pressure/friction dermatitis: localized at edges and bony prominences (malleoli, epicondyles, metacarpal heads) due to folds, sharp edges, or point pressure.
- True allergic reactions: uncommon but may present with intense itch or urticaria-like changes, sometimes in atopic individuals.
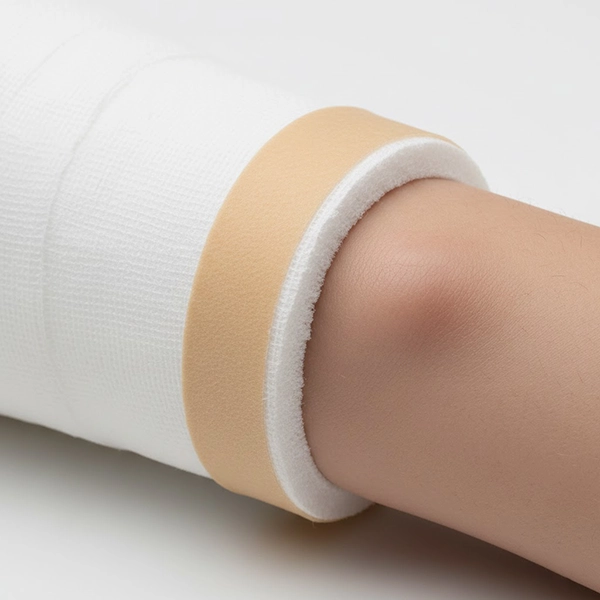
2) Risk factors & structured prevention
- Sensitive/atopic skin: use uniform soft padding; cover edges with moleskin or fabric tape.
- Heat & humidity: increase sweating; keep activation water lukewarm and avoid prolonged soaking.
- Technique: 30–50% overlap, even tension, no folds; reinforce pressure-prone areas; avoid direct contact of wet resin with skin.
- Consumables: fresh, supple rolls (stored 15–30 °C, RH<60%); low-MVTR pouches with clear LOT/EXP.
3) Red flags that warrant review
- Persistent intense itch, foul odor, discharge, or visible staining
- Escalating pain, progressive swelling, blistering, or edge ulceration
- Numbness or discoloration of digits (vascular concern—urgent check)
4) Clinical playbook
- Rapid assessment: allergy history, site, onset, severity.
- Edge/pressure review: if sharp edge or point pressure, perform trim & pad; add moleskin.
- Conservative drying: if moisture is suspected, cool-air drying and patient instruction.
- Suspected resin sensitivity: if symptoms persist, consider local windowing/partial replacement while maintaining immobilization; severe cases—full replacement per clinician judgment.
- Supportive care: per clinician: cool compress, mild oral antihistamine, selective topical agents applied only to exposed skin around edges (never under the cast).
5) Patient education (Do & Don’t)
- Clean & dry: keep skin around edges dry; avoid creams/sprays under the cast.
- Itch: never insert objects; use cool-air drying to ease itch.
- Bathing: use a proper waterproof cover; if wet, blot + cool-air dry.
- Timely reporting: promptly report worsening pain, odor, discharge, or numbness.
6) Casting-unit quality checks
- FEFO rotation and suppleness of rolls; chart LOT/EXP
- Controlled activation water temperature and timed molding window
- Periodic refreshers on edge finishing and padding reinforcement

Conclusion & CTA
With proper materials, technique, and patient education, the risks of resin allergy and contact dermatitis with fiberglass casts can be minimized. For case-specific guidance and staff briefing, please contact our team.


